Borderline Personality Disorder (BPD): Types, Symptoms, Causes, and Treatment

Borderline Personality Disorder (BPD) is marked by unstable emotions, difficulty in relationships, and a fluctuating sense of self. BPD manifests in several types, including Impulsive BPD, Discouraged BPD, Self-Destructive BPD, and Petulant BPD, defined by mood swings and irritability.
As a type of Cluster B personality disorder, BPD is characterized by key symptoms such as unstable relationships, self-harming behaviors, intense fear of abandonment, unstable self-image, impulsive actions, chronic emptiness, fierce anger, and transient stress-related paranoia, according to a study by Skodol et al. 2002, “The borderline diagnosis I: psychopathology, comorbidity, and personality structure.” These symptoms create significant emotional turmoil and difficulties in daily functioning.
The causes of BPD are complex, involving genetic predispositions, environmental factors like childhood trauma, and neurological abnormalities, according to a book by Chapman J, Jamil RT, Fleisher C, et al. 2024, “Borderline Personality Disorder.” The study indicates that a combination of these elements contributes to the development of the disorder, affecting emotional regulation and behavior.
Treatment for BPD includes psychotherapy, such as Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT), which help manage symptoms and improve coping skills, according to a study by Biskin RS, Paris J. et al. 2012, “Management of borderline personality disorder.” Medication addresses specific symptoms, and support from family therapy and support groups is beneficial in treating Borderline Personality Disorder.
What is Borderline Personality Disorder (BPD)?
Borderline Personality Disorder (BPD) is a severe mental health condition characterized by pervasive instability in moods, behavior, self-image, and functioning. Borderline Personality Disorder (BPD) disorder results in impulsive actions and unstable relationships. BPD is defined by a pattern of instability in interpersonal relationships, self-image, and affects, along with marked impulsivity that begins by early adulthood and is present in a variety of contexts, according to the report of Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5),
The DSM-5 outlines nine criteria for diagnosing BPD, with the presence of at least five needed for a diagnosis, according to an article by Biskin RS, Paris J. et al. 2012, “Diagnosing borderline personality disorder.”
These criteria include frantic efforts to avoid real or imagined abandonment, a pattern of unstable and intense interpersonal relationships characterized by alternating between extremes of idealization and devaluation, identity disturbance, impulsivity in at least two areas that are potentially self-damaging, recurrent suicidal behavior or self-mutilating behavior, affective instability due to a marked reactivity of mood, chronic feelings of emptiness, inappropriate, intense anger or difficulty controlling anger, and transient, stress-related paranoid ideation or severe dissociative symptoms.
Approximately 1.4% of the adult population is diagnosed with BPD, according to a report by the National Alliance on Mental Illness in the United States. BPD disorder is more commonly diagnosed in women, accounting for about 75% of the cases.
However, some experts believe it is equally prevalent among men but misdiagnosed as other conditions like post-traumatic stress disorder (PTSD) or depression. Specifically, in New Jersey, BPD’s prevalence is consistent with national statistics, with around 1.2% of the population suffering from Borderline personality disorder.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
More Resources on Addiction:
What are the Types of Borderline Personality Disorder?
The types of Borderline Personality Disorder (BPD) are impulsive behaviors, pervasive discouragement, self-destructive tendencies, and petulant reactions.

The following are the 4 types of borderline personality disorder:
Impulsive BPD
Impulsive BPD is defined by a pattern of impulsivity and risky behaviors. Individuals with this type of borderline personality disorder frequently engage in spontaneous actions without considering potential consequences, such as reckless driving, substance abuse, or unsafe sexual activities, according to a study by Martin S, Del-Monte J, Graziani P., et al. 2019, “Impulsivity issues in borderline personality disorder and it’s linked with insight: the role of urgency.
” Impulsive behaviors stem from a desire for excitement and avoidance of boredom, leading to unstable relationships and significant personal and professional difficulties. Martin studied 81 women with Borderline Personality Disorder (BPD) and assessed their level of insight and impulsivity using two scales: the Beck Cognitive Insight Scale and the UPPS-Short Form Scale.
His findings revealed that while negative emotions, such as anger, anxiety, and grief, significantly impact the quality of insight, positive feelings like happiness, excitement, contentment, and curiosity also play a surprising role in clinical insight. Impulsivity in BPD is frequently associated with abnormalities in the brain’s frontal lobe, which is responsible for decision-making and impulse control.
Discouraged BPD
Discouraged BPD, also known as quiet BPD, is characterized by dependency and passivity. Individuals with this type of borderline personality disorder internalize their emotions, resulting in feelings of emptiness and helplessness.
They depend heavily on others for validation and support while fearing abandonment and rejection, as noted by a case report by Duică L, Antonescu E, Totan M, Boța G, Silișteanu SC. et al. 2022, “Borderline Personality Disorder “Discouraged Type”: A Case Report.” The case study describes an 18-year-old female with a complex psychiatric history, initially diagnosed with major depressive disorder and OCD. Her symptoms, including severe anxiety, psychosis, and social withdrawal, evolved, leading to a diagnosis of Borderline Personality Disorder (BPD) with a discouraged type. This subtype of BPD is characterized by a pattern of dependency, passivity, and self-doubt linked to perfectionism and social inhibition.
Despite initial improvements with treatment, the patient continued to struggle with impaired functionality and self-image issues. The case highlights the challenges of diagnosing discouraged BPD and its overlap with perfectionism, underscoring the need for careful evaluation to avoid misdiagnosis.
Self-Destructive BPD
Self-Destructive BPD is defined by behaviors that are harmful to oneself, including self-injury, suicidal ideation, and disordered eating. Individuals with this type engage in self-harm as a means to cope with emotional pain or to exert a sense of control. This form of BPD is particularly hazardous due to the high risk of suicide, according to a study by Gallop R. et al. 1992, “Self-destructive and impulsive behavior in the patient with a borderline personality disorder: Rethinking hospital treatment and management.” Approximately 10% of individuals with BPD die by suicide, underscoring the critical need for effective intervention and support, according to a study by Paris J et al. 2019, “Suicidality in Borderline Personality Disorder.”
Petulant BPD
Petulant BPD is characterized by intense mood swings, irritability, and difficulty managing anger. Individuals with this type feel misunderstood and unappreciated, leading to bitterness and resentment.
They display aggressive behaviors, lashing out at others when feeling slighted or frustrated, according to an article by American Addiction Centers 2024, “Borderline Personality Disorder (BPD): Causes, Types & Treatment.” Petulant BPD severely strains personal and professional relationships. Petulant BPD is associated with dysregulation in the brain’s limbic system, which is crucial for emotional processing and response, as studied by Silk KR. et al. 2010, “The quality of depression in borderline personality disorder and the diagnostic process.”
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your mental health journey, we are here to help.
What are the Symptoms of Borderline Personality Disorder?
The symptoms of Borderline Personality Disorder (BPD) are characterized by a pattern of unstable moods, self-image, and relationships, including intense and fluctuating emotions, impulsive behaviors, and a distorted self-image.
The key symptoms of Borderline personality disorder are:
Intense and Unstable Relationships
Intense and unstable relationships refer to interactions characterized by extreme fluctuations in idealization and devaluation of others, which lead to tumultuous and conflicted relationships. In Borderline Personality Disorder (BPD), this symptom manifests through rapidly shifting perceptions of others, where individuals alternate between viewing someone as perfect and then as completely flawed.
This instability creates significant relational turmoil with friends, family, and partners. Instability in relationships is a core feature of BPD, as mentioned in a study by Skodol et al. 2002, “The borderline diagnosis I: psychopathology, comorbidity, and personality structure.” The research article examines the psychopathology, comorbidity, and personality structure of Borderline Personality Disorder (BPD), highlighting its severe impact, including high functional impairment and suicide risk.
Self-Harming Behaviors
Self-harming behaviors involve deliberate actions that inflict physical harm on oneself as a means to cope with or express emotional pain. For individuals with BPD, self-harm serves as a response to intense feelings of emptiness, anger, or distress.
This includes behaviors such as cutting, burning, or hitting oneself, according to a review by Zanarini et al. 2008, “The 10-year course of physically self-destructive acts reported by borderline patients and axis II comparison subjects.” The study tracked physically self-destructive behaviors in 290 borderline patients and 72 comparison subjects with Axis II disorders, as categorized by DSM, which includes Personality Disorders and Mental Retardation. The research revealed that while borderline patients initially reported high rates of self-mutilation and suicide attempts, these behaviors decreased significantly over the ten years.
Despite the reduction, borderline patients continued to exhibit higher rates of these behaviors compared to Axis II comparison subjects. At baseline, most borderline patients had a history of both types of self-destructive actions, but by the fifth follow-up, these behaviors had notably diminished, reflecting a shift from severe to less frequent patterns.
Fear of Abandonment
Fear of abandonment is characterized by an intense and pervasive anxiety about being abandoned or left alone, resulting in frantic efforts to avoid separation. In BPD, this fear drives individuals to engage in behaviors aimed at preventing real or perceived abandonment, such as clinging or rapidly forming new relationships.
A study by Palihawadana V et al. 2019, “Reviewing the clinical significance of ‘fear of abandonment’ in borderline personality disorder.” The literature review and case study illustrate that this fear leads to extreme emotional responses and self-destructive behaviors, deeply affecting interpersonal relationships and clinical management. Despite its prominence, existing therapies address this fear indirectly, and specific interventions targeting abandonment are lacking.
Unstable Self-Image
Unstable self-image refers to a fluctuating and inconsistent sense of self where individuals struggle to maintain a stable self-identity. In the context of BPD, individuals experience dramatic shifts in self-perception and self-esteem, leading to changes in goals, values, and career plans, according to research by Westen et al. 2004, “Identity disturbance in adolescence: Associations with borderline personality disorder.” Researchers used a special questionnaire to identify four main identity problems in adolescents: uncertainty about who they are, getting too caught up in roles, feeling confused about themselves, and inconsistent behavior. The study found that these identity issues are significant and linked to serious personality disorders, suggesting that identity problems in teens indicate deeper psychological issues beyond normal teenage struggles.
Rediscover Life at White Light Behavioral Health
Get the compassionate support you deserve. We're here to help you reclaim joy, wellness, and a brighter future.

Impulsive Behaviors
Impulsive behaviors are actions taken without forethought, resulting in harm or regret. Individuals with BPD frequently exhibit impulsive behaviors, such as substance abuse, reckless driving, binge eating, or unsafe sexual practices.
This impulsivity significantly impacts their daily functioning and emotional stability, according to a study by Linehan et al. 2006, “Two-year randomized controlled trial and follow-up of dialectical behavior therapy vs therapy by experts for suicidal behaviors and borderline personality disorder.” In this study, 101 women with borderline personality disorder (BPD) who had recently engaged in self-injury or suicidal behaviors were treated with either Dialectical Behavior Therapy (DBT) or community treatment by experts for one year. The study found that DBT led to better outcomes compared to community treatment.
Women in the DBT group were less likely to attempt suicide, needed fewer hospitalizations, and had lower medical risks. They also stayed in treatment longer and had fewer psychiatric emergencies.
Chronic Feelings of Emptiness
Chronic feelings of emptiness involve a persistent sense of emotional void or lack of fulfillment. For those with BPD, these feelings of emptiness contribute to difficulties in forming meaningful connections and experiencing life satisfaction, according to a study by Miller CE, Townsend ML, et al. 2021, “Understanding chronic feelings of emptiness in borderline personality disorder: a qualitative study.” This study explored the experience of chronic emptiness in people with Borderline Personality Disorder (BPD) through interviews with 15 participants.
It found that chronic emptiness in BPD is characterized by a profound sense of disconnection from oneself and others, accompanied by feelings of numbness and purposelessness. Participants described emptiness as frequent and distressing, impacting their functional capacity.
While they distinguished it from loneliness, hopelessness, dissociation, and depression, they responded to it through either impulsive behaviors or adaptive coping strategies.
Intense Anger
Intense anger is characterized by extreme and uncontrollable rage that is disproportionate to the triggering situation. In BPD, intense anger manifests through frequent outbursts or rage episodes, leading to interpersonal conflicts and self-harm.
Managing anger is particularly challenging for individuals with BPD, affecting their relationships and emotional regulation, according to a study by Neukel C, Bullenkamp R., et al. 2022, “Anger instability and aggression in Borderline Personality Disorder – an ecological momentary assessment study.” This study looked at how anger and aggression affect people with Borderline Personality Disorder (BPD) in their daily lives. It found that people with BPD have more ups and downs with their anger compared to those without BPD. On days when they acted aggressively, their rage was both stronger and more unstable.
This suggests that both high and fluctuating anger leads to aggressive behavior.
Transient Stress-Related Paranoia
Transient stress-related paranoia involves brief episodes of paranoia or severe dissociation occurring during periods of heightened stress. Individuals with BPD experience paranoia or a sense of detachment from reality during episodes of emotional distress. While these symptoms are temporary, they significantly impact daily functioning and interpersonal interactions, according to an article by Freed B. et al. 2022, “Borderline Personality Disorder and Psychosis: A Case Managed by Transference-Focused Psychotherapy.”
What are the Causes of Borderline Personality Disorder?
The causes of Borderline Personality Disorder (BPD) are multifaceted and involve a combination of genetic, environmental, and neurological factors. BPD emerges from an interplay of these influences, though the precise mechanisms remain complex and not fully understood, according to a book by Chapman J, Jamil RT, Fleisher C, et al. 2024, “Borderline Personality Disorder.”
The key causes of BPD include genetics, environmental factors, and changes in brain function, as discussed below:
- Genetic Factors: Genetic factors refer to the hereditary traits and genetic predispositions passed down through family lineage that influence the development of mental health disorders. Borderline personality disorder (BPD) has a genetic component, meaning it tends to run in families, according to a study by Torgersen S. et al. 2000, “Genetics Of Patients With Borderline Personality Disorder.” Genetic factors contribute to approximately 60% of the risk.
- Environmental Factors: Environmental factors pertain to the external conditions and life experiences that shape an individual’s mental health.
Specifically, traumatic experiences during childhood, such as abuse, neglect, or exposure to dysfunctional family dynamics, are strongly linked to the development of BPD, according to a review by Zanarini MC et al. (2011), titled “Childhood Adversity and the Development of Borderline Personality Disorder,” The adverse experiences severely disrupt emotional development and contribute to the manifestation of BPD symptoms. The study highlights that about 70% of individuals with BPD report having experienced severe childhood trauma, emphasizing how early life adversities are crucial in the disorder’s development.
- Neurological Factors: Neurological factors involve abnormalities in brain structure and function predisposing individuals to mental health conditions.
In the context of BPD, these factors include structural and functional changes in brain regions responsible for emotional regulation and impulse control, according to research by Schmahl DG et al. 2003, titled “Magnetic resonance imaging of hippocampal and amygdala volume in women with childhood abuse and borderline personality disorder.” This study on borderline personality disorder (BPD) used MRI to measure the sizes of the hippocampus and amygdala in women with BPD compared to healthy controls. The results showed that individuals with BPD had, on average, 21.9% smaller amygdala volumes and 13.1% smaller hippocampal volumes than those without the disorder.
Are you covered for treatment?
White Light Behavioral Health is an approved provider for Blue Cross Blue Shield and TUFTS, while also accepting many other major insurance carriers.
Check Coverage Now!What are the Risk Factors for Developing Borderline Personality Disorder?
The risk factors for developing Borderline Personality Disorder (BPD) include a combination of genetic predispositions, early life experiences, and certain psychological traits.
The primary risk factors for BPD are:
- Family History of BPD: It refers to having close relatives, such as parents or siblings, who have been diagnosed with borderline personality disorder. Such a family history increases the likelihood of developing BPD due to genetic predispositions, according to a study by Torgersen S. et al. 2000, “Genetics Of Patients With Borderline Personality Disorder.” Genetic factors contribute to approximately 60% of the risk.
- Childhood Trauma: Childhood trauma encompasses severe experiences of abuse or neglect during early development, including physical, emotional, or sexual abuse.
Experiencing these traumatic events significantly heightens the risk of developing BPD. The impact of such early adverse experiences disrupts emotional development and contributes to the development of BPD symptoms.
- Emotional Instability: Emotional instability is characterized by heightened sensitivity to emotional experiences and difficulty managing emotions. Emotionally unstable individuals experience intense and fluctuating emotions that lead to problems in interpersonal relationships and self-regulation, according to a literature review by D’Aurizio G, Di Stefano R, Socci V, et al. 2023, “The role of emotional instability in borderline personality disorder: a systematic review.” The study reviewed 120 research papers on emotional instability and borderline personality disorder (BPD), finding that emotional instability is closely linked to BPD. Out of these, 11 studies met the criteria and were included in the review.
The results show that emotional instability not only worsens BPD symptoms but is also a key factor in the disorder’s development. This suggests that problems with emotional regulation could play a significant role in both the onset and progression of BPD.
- Dysfunctional Family Environment: A dysfunctional family environment refers to growing up in a home characterized by instability, conflict, or unhealthy dynamics.
Such an environment impairs emotional development and contributes to the risk of developing BPD, according to a study by Malik MN et al. 2023, “Borderline Personality Traits, Dysfunctional Family and Risk-Taking Behaviors in Prison Inmates.” The study suggests that factors such as ongoing conflict, inconsistent parenting, or lack of emotional support disrupt the development of healthy emotional regulation skills, making individuals more vulnerable to BPD.
- Personality Traits: Personality traits are enduring characteristics that influence behavior and emotional responses. Traits such as impulsivity and extreme sensitivity make individuals more susceptible to BPD and worsen its symptoms, according to an article by Chapman J, Jamil RT, Fleisher C, et al. 2024, “Borderline Personality Disorder.” The article suggests that 4 or more of the following personality traits must be present: emotional lability, anxiousness, separation insecurity, depressivity, impulsivity, risk-taking, or hostility to risk the development of Borderline Personality Disorder.
Who is at Risk for Borderline Personality Disorder?
Individuals at risk for Borderline Personality Disorder (BPD) include those with a family history of the disorder, as genetic factors greatly increase susceptibility.
People who have experienced severe childhood trauma, such as physical, emotional, or sexual abuse, are also at higher risk due to the long-term impact of these early adverse experiences on emotional regulation and interpersonal relationships.
Additionally, individuals with a history of emotional instability, including those who struggle with intense emotional responses and difficulty managing their feelings, are more prone to developing BPD. Those who have grown up in dysfunctional family environments characterized by instability, conflict, or neglect are also at a heightened risk.
Moreover, individuals displaying certain personality traits, such as impulsivity and heightened sensitivity, are more vulnerable to developing BPD, as these traits exacerbate symptoms and affect emotional regulation.
How is BPD Diagnosed?
To diagnose Borderline Personality Disorder (BPD), a comprehensive evaluation by a qualified mental health professional is required. The diagnosis process includes a detailed clinical interview, during which the clinician assesses the individual’s symptoms, medical history, and family history of mental health issues, according to the study by Tragesser SL, Solhan M., et al. 2014, “Longitudinal associations in borderline personality disorder features: Diagnostic Interview for Borderlines-Revised (DIB-R) scores over time.” During this assessment, the professional will use standardized diagnostic tools and questionnaires to understand the individual’s emotional and behavioral patterns thoroughly.
Tragesser used the Revised Diagnostic Interview for Borderlines (DIB-R) to assess 353 young adults ages 18 and 20 to determine which aspects of borderline personality disorder (BPD) were best at predicting future BPD features. It compared three models: one focusing on affect (emotional state), another on impulse action patterns, and a combined model.
The findings showed that affect scores were the strongest predictor of future BPD symptoms, while impulsivity was less well predicted by affect alone.
According to the DSM-5, the diagnosis of BPD is based on specific criteria outlined in the manual. To be diagnosed with BPD, an individual must exhibit a pervasive pattern of instability in interpersonal relationships, self-image, and affect, along with marked impulsivity. This pattern must be evident across various contexts, leading to significant distress or impairment. The DSM-5 lists nine criteria for BPD, and a diagnosis is made if an individual meets at least five of these criteria, according to an article by Biskin RS, Paris J. et al. 2012, “Diagnosing borderline personality disorder.” These criteria include symptoms such as intense and unstable relationships, fear of abandonment, identity disturbance, and impulsivity.
What are the Treatment Options for Borderline Personality Disorder (BPD)?
The treatment options available for Borderline Personality Disorder (BPD) encompass a range of therapies and medication interventions designed to manage symptoms and improve overall well-being, including psychotherapy, medication, hospitalization, and alternative therapies.
The main treatment options for borderline personality disorder, according to a study by Biskin RS, Paris J. et al. 2012, “Management of borderline personality disorder,” are as follows:
- Psychotherapy: Psychotherapy, or talk therapy, is a primary treatment method for Borderline Personality Disorder (BPD) that involves structured conversations between a patient and a trained therapist. Common types include Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), and Schema-Focused Therapy.
These therapeutic approaches help individuals with BPD by improving their understanding of emotions, enhancing interpersonal skills, and developing effective coping strategies. While recovery time varies, many people start to see improvements within a few months of consistent therapy, according to the study by Biskin.
The main advantage of psychotherapy is its focus on long-term skill development and emotional regulation. However, it requires a significant time commitment and is intensive.
- Medication: Medication refers to the use of pharmaceutical drugs to manage symptoms of BPD, such as mood swings, depression, or anxiety.
Commonly prescribed medications include antidepressants, antipsychotics, and mood stabilizers. These drugs help alleviate some of the symptoms associated with BPD, but they do not cure the disorder itself.
The effectiveness of medication varies, and it takes several weeks to months to notice its full impact, as studied by Biskin. While medication provides relief from specific symptoms, it comes with potential side effects and does not address the root causes of BPD.
- Hospitalization: Hospitalization is a treatment option that provides a controlled environment for individuals experiencing severe symptoms or crises related to BPD. It offers immediate, intensive care and support but is disruptive to daily life.
The length of hospitalization varies based on individual needs and progress. This setting is particularly useful for ensuring safety and stabilizing individuals in acute distress.
- Support Groups: Support groups are gatherings where individuals with BPD come together to share their experiences and provide mutual support.
Support groups offer a space for discussing challenges and coping strategies with peers who have similar experiences, according to Biskin. While support groups provide valuable emotional support and validation, they are not a substitute for formal therapy but complement it by providing additional encouragement and shared understanding.
- Family Therapy: Family therapy involves working with family members to improve understanding and support within the family unit.
It helps address communication issues and enhance relational dynamics, particularly beneficial for individuals with BPD. Family therapy aims to strengthen family support systems and improve overall family functioning, contributing positively to the individual’s treatment.
- Skills Training Programs: Skills training programs focus on teaching practical skills for managing symptoms of BPD. Support and skill development programs cover areas such as emotional regulation, stress management, and interpersonal effectiveness, according to Biskin’s study. They are designed to complement psychotherapy by providing additional tools for managing daily challenges and improving overall functioning.
What is the Difference Between Borderline Personality Disorder and Other Mental Disorders?
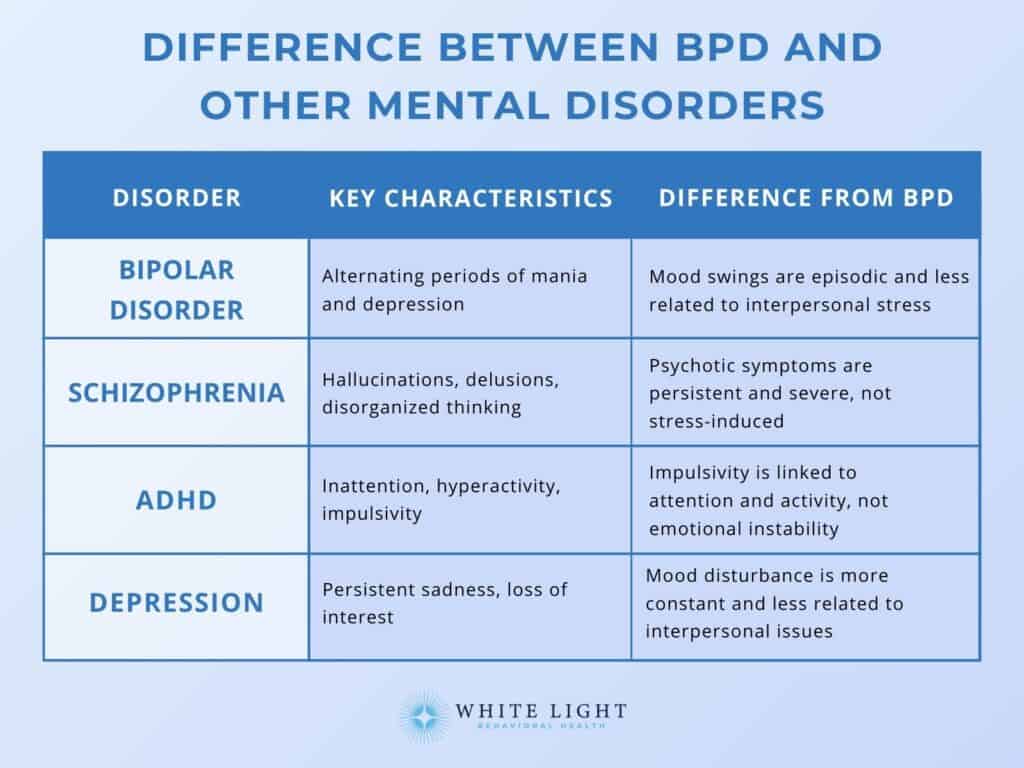
The main difference between Borderline Personality Disorder (BPD) and other mental disorders is that BPD is characterized by pervasive instability in mood, self-image, and interpersonal relationships, whereas other mental disorders focus on specific symptoms like anxiety, depression, or psychosis.
While BPD shares some symptoms with other mental disorders, such as Bipolar Disorder, Schizophrenia, ADHD, and Depression, there are distinct differences that set BPD apart. Emotional instability, impulsive behaviors, and unstable relationships distinguish Borderline Personality Disorder (BPD).
In contrast, Bipolar Disorder features distinct mood episodes of mania and depression, according to an article by Healthline 2023, “Your FAQs Answered: Bipolar Disorder vs. Borderline Personality Disorder.” Schizophrenia involves chronic psychotic symptoms like hallucinations, which are not typical of BPD. ADHD primarily affects attention and hyperactivity, with impulsivity being just one aspect, unlike BPD, where impulsivity is tied to emotional instability.
Depression is marked by a persistent low mood and loss of interest, contrasting with BPD’s mood swings that are triggered by interpersonal issues.
Did you know most health insurance plans cover substance use disorder treatment? Check your coverage online now.
What is the Difference Between Borderline Personality Disorder and Bipolar Disorder?
The primary difference between Borderline Personality Disorder (BPD) and Bipolar Disorder lies in the duration and triggers of mood changes. Although both are mental health conditions that involve mood instability, Bipolar Disorder involves longer-lasting episodes of mania or depression that occur independently of external events, according to an article by Healthline 2023, “Your FAQs Answered: Bipolar Disorder vs. Borderline Personality Disorder.”
Pervasive emotional instability, impulsive behaviors, and intense, unstable relationships mark Borderline Personality Disorder (BPD). Individuals with BPD experience rapid mood swings, but these are usually triggered by interpersonal stressors or perceived abandonment.
Bipolar Disorder, on the other hand, is characterized by extreme mood swings that include manic or hypomanic episodes and depressive episodes. These mood changes are more episodic and less related to immediate interpersonal stressors than in BPD.
What is the Difference Between Borderline Personality Disorder and Schizophrenia?
The key difference between BPD and Schizophrenia lies in psychotic experiences. BPD’s transient psychotic-like symptoms are stress-induced, while schizophrenia involves more persistent and severe psychotic features, according to a comparative study by Kingdon DG. et al. 2010, “Schizophrenia and borderline personality disorder: similarities and differences in the experience of auditory hallucinations, paranoia, and childhood trauma.” This study compared experiences of auditory hallucinations, paranoia, and childhood trauma in patients with schizophrenia and Borderline Personality Disorder (BPD).
It found that while both groups had similar experiences with auditory hallucinations, BPD patients, including those with comorbid schizophrenia, reported higher levels of childhood trauma, particularly emotional abuse. The study highlights the frequent comorbidity of BPD and schizophrenia and underscores the need for careful assessment and management of childhood trauma in BPD patients.
Borderline Personality Disorder (BPD) is characterized by emotional dysregulation, impulsivity, and unstable interpersonal relationships. Individuals with BPD experience transient psychotic symptoms under stress but maintain a stable sense of reality.
Schizophrenia is a severe mental disorder that includes chronic symptoms such as hallucinations, delusions, and disorganized thinking. Unlike BPD, schizophrenia involves persistent psychotic symptoms that seriously impair an individual’s ability to function in daily life.
What is the Difference Between Borderline Personality Disorder and ADHD?
The main difference between Borderline Personality Disorder (BPD) and ADHD is that BPD primarily involves emotional instability and interpersonal difficulties, while ADHD is characterized by persistent inattention, hyperactivity, and impulsivity.
Attention-Deficit/Hyperactivity Disorder (ADHD) is characterized by persistent patterns of inattention and hyperactivity-impulsivity that are inconsistent with developmental level and interfere with functioning.
While both disorders involve impulsivity, ADHD is primarily focused on attention and activity levels, whereas BPD’s impulsivity is more related to emotional instability and interpersonal relationships, according to an article by Dr. Neff, “ADHD vs BPD.” ADHD symptoms are usually present from childhood, whereas BPD symptoms emerge in late adolescence or early adulthood.
What is the Difference Between Borderline Personality Disorder and Depression?
The main difference between Borderline Personality Disorder (BPD) and Depression is the nature and cause of the mood disturbances. BPD mood swings are related to relational stress and self-image issues, while depression involves more constant and pervasive feelings of sadness, according to a study by Galione JN, Oltmanns TF. et al. 2014, “The relationship between borderline personality disorder and major depression in later life: acute versus temperamental symptoms.”
Borderline Personality Disorder (BPD) is defined by emotional instability, impulsivity, and unstable interpersonal relationships, with an intense fear of abandonment. Individuals with BPD experience mood swings, but these are usually reactive to interpersonal stressors.
Depression, specifically Major Depressive Disorder (MDD), involves persistent feelings of sadness or loss of interest in activities, along with other symptoms like changes in sleep, appetite, and concentration. Unlike BPD, depression is characterized by a more pervasive and consistent low mood that is not necessarily triggered by interpersonal dynamics.
What are the Signs of BPD in Females?
The signs of Borderline Personality Disorder (BPD) in females include intense and unstable relationships marked by fears of abandonment and emotional instability with rapid mood swings. Women with BPD engage in impulsive behaviors, such as substance abuse or self-harm, and experience chronic feelings of emptiness, according to a comparative study by Bozzatello P. et al. 2024, “Gender differences in borderline personality disorder: a narrative review.” Women also exhibit intense anger, difficulty controlling their emotions, and have a fluctuating self-image. These symptoms significantly affect their daily life and relationships.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your mental health journey, we are here to help.
What Triggers BPD?
Triggers for Borderline Personality Disorder (BPD) include interpersonal stress, such as perceived rejection or abandonment, and high emotional stress from conflicts or disappointments, according to a blog by Optimum Performance Institute, 2018, “Borderline Personality Disorder Triggers.” Major life changes and past traumatic experiences also exacerbate symptoms. Understanding these triggers helps in managing the condition more effectively.
What Happens if BPD is Left Untreated?
If Borderline Personality Disorder (BPD) is left untreated, symptoms worsen, leading to severe emotional instability and an increased risk of self-harm or suicide. About 8% to 10% of people with untreated BPD die by suicide, according to an article by Healthline, “Borderline Personality Disorder (BPD).” Many people with untreated BPD also experience unstable or chaotic personal relationships and have trouble keeping a job.
They have an increased risk of divorce, estrangement from family members, and rocky friendships. Legal and financial problems are also common.
Untreated BPD results in chronic relationship issues, social isolation, and the development of other mental health problems like depression or substance abuse. Overall, untreated BPD severely impairs one’s quality of life and ability to function effectively in daily activities.
Share This Post